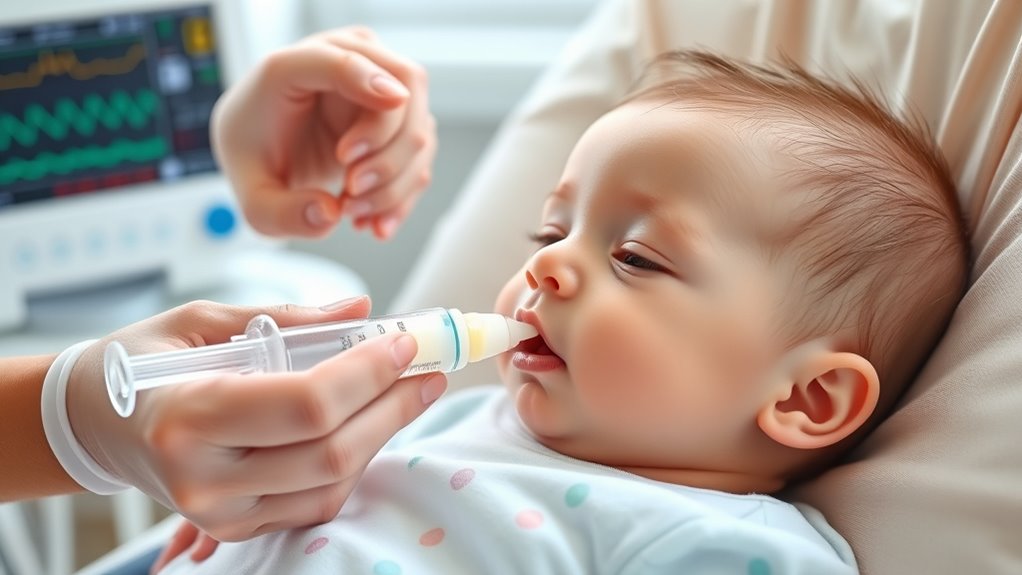
To manage reflux, feed your baby smaller, more frequent amounts and keep them upright at about 45-90 degrees during and after feeds, holding them for 20-30 minutes post-meal. Use slow-flow bottles or adjust breastfeeding to reduce air swallowing. Avoid lying flat immediately after feeding and watch for signs of discomfort or fullness. Experiment with positioning and routines, as each baby responds differently—continuing will help you discover what works best for your little one.
Key Takeaways
- Offer smaller, more frequent feedings to prevent overfeeding and minimize reflux triggers.
- Keep the baby upright at 45-90 degrees during and after feeding for 20-30 minutes.
- Use anti-colic bottles and slow-flow nipples to reduce air swallowing and discomfort.
- Avoid lying flat immediately after feeding; maintain an inclined position to help gravity keep stomach contents down.
- Monitor feeding cues and provide breaks to prevent overfeeding and ease reflux symptoms.
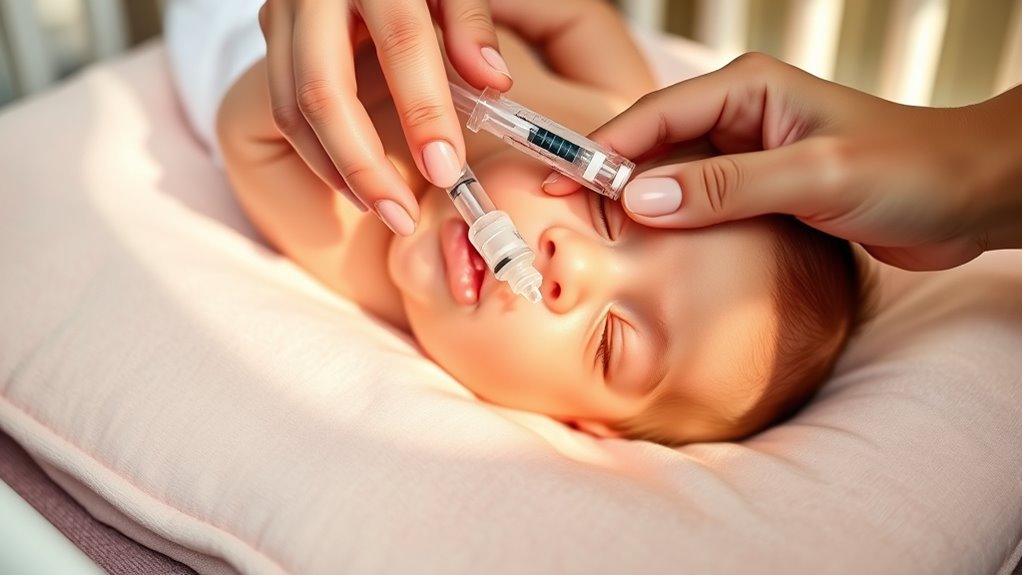
Reflux can make feeding times challenging, but making simple adjustments can markedly reduce discomfort. When your baby experiences reflux, it’s often due to certain reflux triggers that provoke the discomfort, such as overfeeding, lying flat after a meal, or feeding too quickly. By developing effective feeding strategies, you can help minimize these triggers and create a more comfortable feeding experience for your little one. Start by observing your baby’s cues—signs like turning away, fussiness, or rooting can indicate they’re full or overwhelmed. Implementing smaller, more frequent feedings can prevent overfilling their stomach, which is a common reflux trigger. This approach not only reduces pressure on their stomach but also helps in managing reflux symptoms more effectively.
Choosing the right feeding position plays an essential role. Keep your baby upright during feeds, ideally at a 45 to 90-degree angle, to help gravity keep stomach contents down and prevent reflux. After feeding, hold your baby upright for at least 20 to 30 minutes, as lying flat can exacerbate reflux symptoms. Using pillows or specialized infant seats that support an inclined position can help maintain this posture comfortably. If you’re breastfeeding, consider adjusting your latch to ensure your baby is swallowing less air, which can contribute to reflux. For bottle-feeding, use anti-colic bottles that reduce air intake and slow the flow rate, helping your baby swallow more calmly and decreasing reflux triggers caused by gulping or swallowing air.
Pay attention to your baby’s feeding routines. Make sure they are calm and alert before starting a feed, as a distressed or overly tired baby may feed too aggressively or swallow air, increasing reflux risk. Also, watch the type of formula or milk you give, as some formulas are designed to be gentler on sensitive stomachs, potentially reducing reflux triggers. If you suspect certain foods in your diet are affecting your breastfeeding baby, consult your healthcare provider about possible adjustments. Additionally, proper burping techniques can help release trapped air and reduce reflux episodes.
Lastly, avoid rushing feedings or pressuring your baby to eat more than they want. Allow them to take breaks if needed, and watch for signs of fullness. This mindful approach to feeding helps prevent overfeeding and minimizes reflux triggers. Remember, every baby is different, so it may take some experimentation to find the best feeding strategies that work for your child. By paying close attention to their cues and making thoughtful adjustments, you can substantially ease their discomfort and make feeding a more positive experience for both of you.

Dr. Brown's Anti-Colic Options + Narrow Bottle to Sippy Gift Set with Soft Silicone Sippy Spout, Removable Silicone Handles, Travel Cap and Bottle Brush (Packaging/Brush Color May Vary)
ANTI-COLIC BABY BOTTLE. Anti-Colic internal vent system is clinically proven to reduce colic. Decreases spit-up, burping and gas.
As an affiliate, we earn on qualifying purchases.
As an affiliate, we earn on qualifying purchases.
Frequently Asked Questions
How Long Does Reflux Typically Last in Infants?
Reflux in infants can last from a few weeks to several months, often peaking around 4 months. You can help manage it by adjusting sleep positioning, like keeping your baby upright after feedings, and using proper feeding techniques. These strategies can lessen discomfort and minimize reflux episodes. Remember, every baby is different, so consult your pediatrician if reflux persists or worsens to ensure proper care.
Are There Specific Foods That Worsen Reflux Symptoms?
Certain foods can worsen reflux symptoms because food sensitivities and dietary triggers play a role. Spicy foods, citrus, chocolate, caffeine, and fatty or fried foods are common culprits. Studies show that up to 50% of reflux cases improve when these triggers are avoided. You should monitor your diet closely, as identifying and eliminating specific foods can markedly reduce reflux discomfort and improve your overall well-being.
When Should I See a Doctor About Reflux Concerns?
You should see a doctor if your reflux causes persistent discomfort, worsens despite dietary changes, or affects sleep safety. Seek medical advice promptly if you experience severe symptoms, difficulty swallowing, or if over-the-counter medications aren’t effective. Addressing medication concerns early helps prevent complications. Don’t ignore signs that interfere with daily life or sleep, as proper treatment can improve your comfort and health.
Can Reflux Affect a Baby’s Growth and Development?
Reflux can impact your baby’s growth and development, with studies showing up to 50% of infants affected at some point. If reflux causes frequent discomfort, it might interfere with feeding strategies, leading to poor nutrition. This can delay developmental milestones like sitting or crawling. Monitoring your baby’s feeding patterns and consulting a healthcare professional can help manage reflux, ensuring your little one grows and develops healthily.
Are There Non-Medical Remedies to Alleviate Reflux Symptoms?
Yes, you can try non-medical remedies to ease reflux symptoms. Herbal remedies like chamomile or ginger may help soothe your baby’s stomach, but consult your pediatrician first. Also, focus on feeding techniques—keep your baby upright during and after feeds, offer smaller, more frequent meals, and burp them thoroughly. These approaches can reduce reflux discomfort and promote better digestion without medication.

Baby Feeding Support Wedge Pillow, Infant Nursing Cushion with Gentle Incline for Bottle Feeding and Tummy Time, Portable Lounger Support
1.Gentle Incline Positioning:The angled wedge design supports a natural upright posture during feeding and supervised rest time. Helps…
As an affiliate, we earn on qualifying purchases.
As an affiliate, we earn on qualifying purchases.
Conclusion
Remember, finding the right feeding routine for reflux can be a gentle journey. By making small adjustments and listening carefully, you create a soothing environment that helps your little one thrive. Sometimes, a subtle change can work wonders, like a quiet whisper guiding you toward comfort. Trust your instincts and be patient—each gentle step brings you closer to smoother days. In time, these gentle shifts will help nurture a calm, happy feeding experience for both of you.

Dr. Brown's Natural Flow Level 1 Narrow Baby Bottle Silicone Nipple, Slow Flow, 0m+, 100% Silicone Bottle Nipple, 6 Count (Pack of 1)
NEWBORN NIPPLE. Dr. Brown's Slow Flow Nipple offers a flow perfect for newborns.
As an affiliate, we earn on qualifying purchases.
As an affiliate, we earn on qualifying purchases.
XFaa Rootling Baby Feeding Pillow, Anti Overflow Feeding Pillow for Reducing Spit-Up, Safety Nursing Pillow, Baby Lounger Reflux Wedge Breastfeeding, Removable top and Bottom
【Dual-Function Detachable Design】: The removable wedge segment transforms this pillow into a flat surface when detached, eliminating the…
As an affiliate, we earn on qualifying purchases.
As an affiliate, we earn on qualifying purchases.